History of TMS (Part 7)
Milestones in TMS Research and Application
Since its FDA approval in 2008, transcranial magnetic stimulation (TMS) has evolved significantly, expanding its clinical applications and improving treatment strategies. Advancements in technology, clinical research, and personalized protocols have helped solidify TMS as a widely accepted therapy for psychiatric and neurological disorders.
This section highlights key milestones in TMS research, focusing on major breakthroughs in treatment precision, efficacy validation, and expanding clinical applications.
2010s: Adoption of Neuronavigation-Guided TMS
One of the most significant advancements in TMS treatment was the integration of neuronavigation systems, which use real-time neuroimaging (MRI, fMRI, or EEG) to precisely locate and target specific brain regions during TMS sessions.
Why Is Neuronavigation Important?
- Traditional TMS relies on external scalp measurements to position the coil, which can be inaccurate due to individual brain variability.
- Neuronavigation increases targeting precision, ensuring that the correct brain region receives consistent stimulation.
- Research has demonstrated that neuronavigation-guided TMS improves clinical outcomes, particularly in treatment-resistant depression (Lisanby, 2017).
Today, many TMS clinics worldwide utilize neuronavigation to personalize treatment protocols, leading to higher response rates and better treatment consistency.
2017: Large-Scale Meta-Analysis Confirms TMS Efficacy for Depression
A major milestone in TMS research was the 2017 publication of a large-scale meta-analysis, which consolidated data from multiple randomized controlled trials (RCTs) to evaluate TMS’s effectiveness for treatment-resistant depression (TRD).
Key Findings of the Meta-Analysis:
✔ TMS significantly reduces depressive symptoms in patients who do not respond to medication.
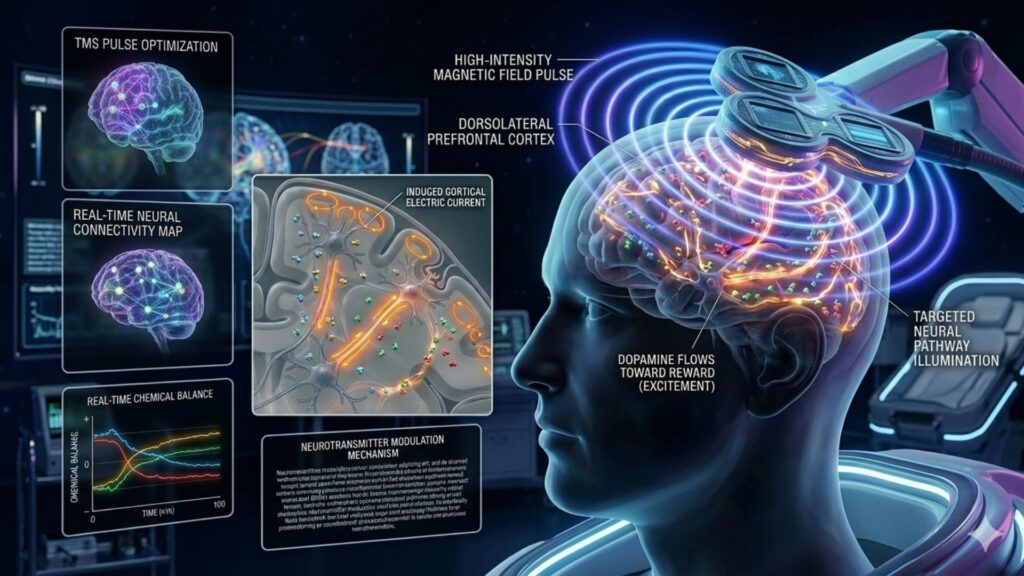
✔ High-frequency rTMS over the left dorsolateral prefrontal cortex (DLPFC) is the most effective protocol.
✔ TMS has a favorable safety profile compared to antidepressant medications, with minimal side effects.
This analysis played a crucial role in validating TMS as a first-line treatment for TRD, leading to increased clinical adoption and insurance coverage (Fitzgerald 2020).
2020s: Expanding TMS Applications Through Clinical Trials
While TMS was originally approved for depression and migraine, ongoing research in the 2020s has expanded its potential applications to neurological and psychiatric conditions, including:
1. PTSD (Post-Traumatic Stress Disorder)
- Ongoing trials are testing TMS over the right prefrontal cortex to modulate emotional processing circuits in PTSD patients.
- Early studies suggest that TMS can reduce hyperarousal and intrusive thoughts, improving PTSD symptoms.
2. Schizophrenia
- Researchers are exploring low-frequency rTMS on the left temporoparietal cortex to reduce auditory hallucinations in schizophrenia.
- Some studies indicate that TMS can improve cognitive deficits and negative symptoms in schizophrenia patients.
3. Bipolar Disorder
- Clinical trials are evaluating whether TMS can stabilize mood in bipolar patients, reducing depressive and manic episodes.
- Early results show potential benefits of TMS for bipolar depression but emphasize the need for personalized protocols.
4. Chronic Pain & Fibromyalgia
- Studies suggest that TMS over the motor cortex can reduce pain perception, offering a non-opioid alternative for chronic pain management.
- Ongoing trials are testing repetitive TMS (rTMS) and theta burst stimulation (TBS) for fibromyalgia and neuropathic pain.
These research efforts demonstrate the growing versatility of TMS, with potential future FDA approvals for a broader range of conditions (Lisanby, 2017).
2023–2024: Innovations in Personalized TMS
Recent advancements have focused on individualizing TMS treatments, moving toward a personalized medicine approach:
1. AI-Driven TMS Targeting
- Artificial intelligence (AI) and machine learning algorithms are being integrated with TMS to identify optimal brain targets for each patient.
- AI-assisted neuronavigation is improving treatment precision and response rates.
2. QEEG-Guided TMS
- Quantitative EEG (QEEG) is being used to map patients’ brain activity patterns before TMS treatment.
- QEEG data helps customize stimulation parameters, leading to better outcomes in depression and anxiety disorders.
3. Accelerated TMS Protocols
- The Stanford SAINT protocol has shown that multiple TMS sessions per day can significantly reduce depression symptoms within 5 days instead of the standard 6-week course.
- Ongoing trials are testing accelerated TMS for PTSD, OCD, and chronic pain.
These innovations are making TMS more efficient, effective, and accessible, setting the stage for future breakthroughs in neuromodulation.
Future Directions in TMS Research
As TMS continues to evolve, several new research areas are shaping its future:
✔ TMS for Cognitive Enhancement – Studies are investigating TMS’s ability to improve memory, attention, and executive function in healthy individuals and patients with Alzheimer’s disease.
✔ TMS & Psychedelic-Assisted Therapy – Researchers are exploring whether TMS can enhance neuroplasticity when combined with psychedelic-assisted psychotherapy.
✔ Home-Based TMS Devices – Clinical trials are testing portable, wearable TMS devices for at-home depression treatment, potentially making TMS more accessible to rural and underserved populations.
With ongoing advancements, TMS is becoming a cornerstone of non-invasive brain stimulation, with the potential to redefine psychiatric and neurological treatments in the coming years.
Conclusion
The milestones in TMS research and application reflect the rapid evolution of this technology from a research tool to a mainstream medical treatment. Key developments such as neuronavigation, large-scale meta-analyses, expanding clinical applications, and personalized TMS approaches have transformed TMS into a powerful, evidence-based therapy.
As new clinical trials explore innovative uses for TMS, its role in neuromodulation, mental health, and neurology is expected to continue growing, making it one of the most promising treatments of the future.
Sources:
- Sack, A. T., Cohen Kadosh, R., Schuhmann, T., Moerel, M., Walsh, V., & Goebel, R. (2009). Optimizing functional accuracy of TMS in cognitive studies: A comparison of methods. Journal of Cognitive Neuroscience, 21(2), 207–221. https://doi.org/10.1162/jocn.2009.21126
- Fitzgerald, P. B. (2020). An update on the clinical use of repetitive transcranial magnetic stimulation in the treatment of depression. Journal of Affective Disorders, 276, 90–103. doi: 10.1016/j.jad.2020.06.067. Epub 2020 Jul 15. PMID: 32697721. https://pubmed.ncbi.nlm.nih.gov/32697721/
- Lefaucheur, J. P., Aleman, A., Baeken, C., Benninger, D. H., Brunelin, J., Di Lazzaro, V., Filipović, S. R., Grefkes, C., Hasan, A., Hummel, F. C., Jääskeläinen, S. K., Langguth, B., Leocani, L., Londero, A., Nardone, R., Nguyen, J. P., Nyffeler, T., Oliveira-Maia, A. J., Oliviero, A., … Ziemann, U. (2020). Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS): An update (2014–2018). Clinical Neurophysiology, 131(2), 474–528. doi: 10.1016/j.clinph.2019.11.002. https://doi.org/10.1016/j.clinph.2019.11.002
- Erickson, M. (2021). Experimental depression treatment is nearly 80% effective in controlled study. Stanford Medicine News Center, published Oct. 29, 2021. Details rapid remission (~79%) using Stanford accelerated intelligent neuromodulation therapy (SAINT). https://med.stanford.edu/news/all-news/2021/10/depression-treatment.html