Palmier TMS Podcast Series: What is TMS Part 5
The Science of Neuroplasticity and TMS
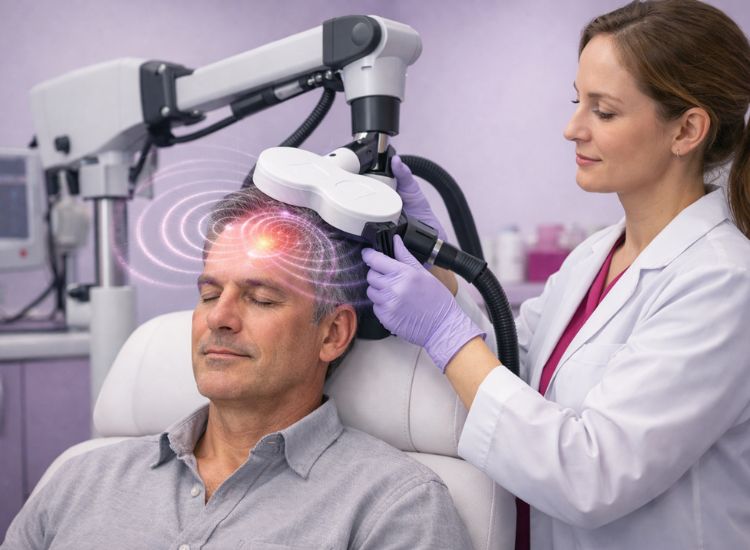
Neuroplasticity refers to the brain’s ability to adapt and reorganize itself by forming new neural connections. This fundamental property allows the brain to recover from injuries, learn new skills, and adapt to changes in the environment. Transcranial Magnetic Stimulation (TMS) leverages neuroplasticity by stimulating areas of the brain associated with mood and cognition, effectively reshaping neural circuits to improve mental health outcomes.
How TMS Influences Neuroplasticity
TMS operates by delivering repeated magnetic pulses to targeted brain regions, such as the dorsolateral prefrontal cortex (DLPFC), an area commonly associated with emotional regulation and cognitive processing. These pulses induce electrical activity in neurons, strengthening or weakening synaptic connections depending on the stimulation frequency.
- High-frequency TMS (≥5 Hz) increases cortical excitability, promoting synaptic potentiation, which strengthens neural connections and enhances activity in underactive brain regions.
- Low-frequency TMS (≤1 Hz) reduces neural excitability, helping to quiet hyperactive circuits that may contribute to mental health disorders.
By modulating these excitatory and inhibitory pathways, TMS restores balance in the brain, mitigating symptoms of conditions like depression, anxiety, and obsessive-compulsive disorder (OCD). These neuroplastic changes can lead to sustained improvements, as the brain continues to reorganize and optimize its function long after treatment concludes.
Strengthening Existing Neural Pathways and Forming New Ones
Repeated stimulation via TMS not only strengthens pre-existing neural pathways but also promotes the formation of new ones. This ability is crucial for patients with psychiatric disorders, as it allows the brain to compensate for dysfunctional circuitry. The mechanism behind these effects lies in:
- Long-term potentiation (LTP): This process strengthens synaptic connections, making neural communication more efficient. It is a key mechanism in learning and memory, reinforcing frequently used pathways to improve cognitive function and emotional regulation. In the context of TMS, LTP helps establish more effective neural circuits for mood stability and adaptive thought patterns.
- Long-term depression (LTD): This weakens specific pathways to reduce maladaptive signaling, often seen in disorders like OCD and PTSD. LTD plays a crucial role in eliminating unnecessary or harmful neural connections, allowing the brain to recalibrate and suppress overactive or dysfunctional circuits. By reducing excessive neural firing, LTD helps restore balance and improve emotional regulation in affected individuals.
Through these mechanisms, TMS fosters a more adaptive and resilient brain network, providing relief from symptoms and improving overall cognitive function.
Lasting Effects of TMS-Induced Neuroplasticity
One of the most significant advantages of TMS therapy is the persistence of its effects beyond the treatment period. Research indicates that neuroplastic changes induced by TMS can last for months or even years, particularly when combined with complementary therapies such as cognitive-behavioral therapy (CBT) or medication management.
This long-term efficacy is attributed to:
- The strengthening of beneficial neural circuits that support mood regulation and cognitive resilience.
- The ongoing adaptation of the brain to optimized patterns of neural activity.
- The gradual reorganization of networks responsible for emotional processing, stress response, and executive function.
- The role of maintenance TMS sessions, which help reinforce neural changes and extend symptom relief beyond the initial treatment phase.
Studies suggest that 58% of patients who achieve remission after TMS maintain improvements at three months, demonstrating the lasting neuroplastic changes induced by repeated stimulation. These persistent effects highlight how TMS strengthens and reorganizes neural networks, allowing the brain to sustain improved mood regulation and cognitive resilience over time, with some experiencing benefits for many years to come. Additionally, integrating maintenance sessions has been shown to prolong symptom relief, reducing the likelihood of relapses by reinforcing neuroplastic adaptations. The continued stimulation helps solidify newly formed synaptic connections, ensuring that beneficial changes in neural activity remain stable and effective. This underscores the importance of continued monitoring and personalized treatment adjustments to sustain long-term benefits.
Clinical Applications and Future Directions
Neuroplasticity is at the heart of many promising advancements in TMS applications. While the therapy is most commonly used to treat depression, emerging research highlights its potential for other conditions mentioned in previous sections, with specific brain regions targeted for different disorders:
- Post-Traumatic Stress Disorder (PTSD): TMS modulates the hyperactive fear response by targeting the ventromedial prefrontal cortex (vmPFC) and the amygdala, helping reduce symptoms of hyperarousal and intrusive thoughts.
- Stroke Rehabilitation: TMS promotes motor recovery by stimulating the primary motor cortex (M1), which plays a crucial role in movement control and coordination. Targeted stimulation can enhance motor function in stroke survivors by strengthening neural pathways associated with limb mobility.
- Chronic Pain Management: The primary motor cortex (M1) and the dorsolateral prefrontal cortex (DLPFC) are key targets for pain management. Stimulating these regions has been shown to modulate pain perception and improve quality of life for individuals with fibromyalgia, neuropathic pain, and other chronic pain conditions.
- Neurodegenerative Disorders: Research is exploring the effects of TMS on the prefrontal cortex and parietal regions, aiming to slow cognitive decline in conditions like Alzheimer’s disease by enhancing neuroplasticity and improving cognitive function.
By continuing to refine stimulation parameters and personalize treatments based on neuroimaging findings, researchers are working to maximize the effectiveness of TMS in promoting beneficial neuroplastic changes across a wide range of conditions.
Conclusion
The ability of the brain to rewire itself through neuroplasticity is one of its most remarkable features, and TMS harnesses this capability to provide lasting relief from mental health and neurological disorders. By promoting synaptic changes, strengthening beneficial circuits, and encouraging adaptive neural activity, TMS stands as a powerful intervention in modern neuroscience. As research continues to expand, the role of TMS in enhancing neuroplasticity will likely grow, paving the way for even more effective and personalized treatments in the future.
Sources:
Pascual-Leone, A., Walsh, V., & Rothwell, J. (2000). Transcranial magnetic stimulation in cognitive neuroscience–virtual lesion, chronometry, and functional connectivity. Current Opinion in Neurobiology, 10(2), 232-237. https://pubmed.ncbi.nlm.nih.gov/10753803/
Huang, Y. Z., et al. (2005). Theta burst stimulation of the human motor cortex. Neuron, 45(2), 201-206. https://doi.org/10.1016/j.neuron.2004.12.033
Valero-Cabré, A., Amengual, J. L., Stengel, C., Pascual-Leone, A., & Coubard, O. A. (2017). Transcranial magnetic stimulation in basic and clinical neuroscience: A comprehensive review of fundamental principles and novel insights. Neuroscience and Biobehavioral Reviews, 83, 381-404. https://pubmed.ncbi.nlm.nih.gov/29032089/
Hallett, M. (2000). Mechanisms of brain stimulation in TMS. Nature, 406(6792), 147-150. https://www.nature.com/articles/35018000