Palmier TMS Podcast Series: What is TMS Part 2
Understanding Magnetic Fields in Medicine
The foundation of Transcranial Magnetic Stimulation (TMS) lies in the use of magnetic fields to influence brain activity. This scientific principle, rooted in the concept of electromagnetic induction, enables clinicians to modulate neural pathways non-invasively. When the TMS coil emits a magnetic pulse, it penetrates the scalp and induces an electrical current in the brain. This current activates or suppresses neurons, depending on the protocol used, allowing TMS to impact targeted regions of the brain.
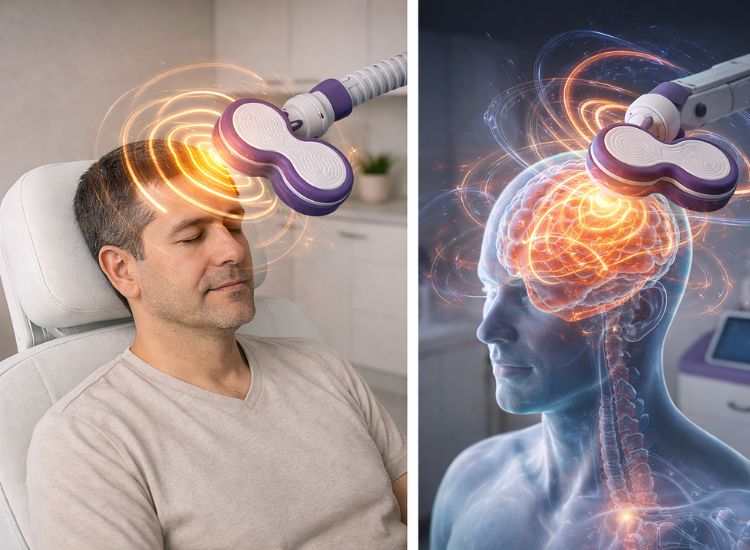
How Magnetic Fields Interact with the Brain
Electromagnetic induction, first discovered by Michael Faraday in the 19th century, is the key mechanism behind TMS. In practice, the TMS coil generates a rapidly changing magnetic field that passes through the skull without resistance. When this magnetic field reaches the brain tissue, it induces a localized electrical current. This current stimulates or inhibits neuronal activity, depending on the frequency and intensity of the magnetic pulses.
The induced current affects the membranes of neurons, altering their resting potential. For instance, high-frequency stimulation (typically above 5 Hz) increases neuronal excitability, activating underactive regions of the brain. Conversely, low-frequency stimulation (around 1 Hz) reduces excitability, suppressing overactive neural activity. These dual effects are a cornerstone of TMS’s versatility.
MRI and TMS: Harnessing Magnetic Fields
MRI technology is widely recognized among the general population and has proven to be a reliable and effective tool in modern medicine. It has revolutionized diagnostic imaging by providing detailed insights into the body’s internal structures, particularly the brain, through the use of electromagnetic fields. Just as MRI has become a cornerstone of medical diagnostics, TMS is emerging as a powerful therapeutic tool, leveraging magnetic fields to influence brain function and treat various neurological and psychiatric conditions.
Similarities Between TMS and MRI in Magnetic Field Use
Although TMS and Magnetic Resonance Imaging (MRI) serve different purposes, both technologies rely on electromagnetic fields to interact with brain tissue in a non-invasive manner. They share key similarities in their fundamental mechanisms:
- Use of Magnetic Fields for Neural Interaction: Both TMS and MRI utilize electromagnetic fields to influence brain activity. While TMS generates magnetic pulses that induce electrical currents in neurons to stimulate or inhibit activity, MRI uses magnetic fields to interact with atomic nuclei in the brain to gather structural and functional data.
- Non-Invasive Approach: Both methods enable clinicians to examine or influence brain activity without requiring surgical intervention. This makes them highly valuable for both research and clinical applications in neurology and psychiatry.
- Precision in Targeting Brain Regions: TMS and functional MRI (fMRI) can be used together to precisely locate and target specific brain regions. MRI can identify structural and functional abnormalities, guiding the placement of the TMS coil for optimized stimulation.
- Magnetic Field Strength and Biological Effects: Although MRI uses a continuous magnetic field while TMS employs rapidly changing pulses, both have been designed to interact safely with brain tissue, ensuring minimal discomfort or adverse effects in patients.
These similarities illustrate the broader role of electromagnetic fields in neuroscience, whether for imaging brain structures or modulating neural activity through TMS.
Promoting Brain Plasticity
One of the remarkable outcomes of TMS is its ability to encourage brain plasticity—the brain’s natural ability to adapt and reorganize neural pathways in response to new experiences. TMS achieves this by strengthening or weakening connections in specific neural circuits, paving the way for long-term improvements in conditions like depression and anxiety. This ability to modulate neural circuits is particularly significant for patients with treatment-resistant conditions, as it provides a means to “reset” disrupted brain activity. Further discussion on neuroplasticity and its role in TMS will be explored in an upcoming chapter.
Focusing on Targeted Brain Regions
A primary focus of TMS therapy is the dorsolateral prefrontal cortex (DLPFC), which is commonly underactive in patients with depression. Stimulating this region fosters healthier communication between neural networks associated with mood and emotional regulation. However, the applications of TMS extend far beyond the DLPFC. For instance:
- Motor Cortex: Often targeted for managing chronic pain and facilitating motor recovery in stroke patients.
- Somatosensory Cortex: Studied for its role in alleviating neuropathic pain.
- Anterior Cingulate Cortex: Linked to emotional regulation, making it a key target for treating anxiety and OCD.
Emerging imaging techniques, such as functional MRI (fMRI) and magnetoencephalography (MEG), are enabling clinicians to map brain activity with greater precision. This allows for more tailored treatments based on each patient’s unique neural patterns, further enhancing outcomes.
Technological Advancements in TMS Protocols
The evolution of TMS technology has significantly enhanced its efficiency and accessibility. Traditional TMS protocols required session durations of 20 to 40 minutes, which could be challenging for patients with busy schedules. However, the development of Theta Burst Stimulation (TBS) has revolutionized this aspect of TMS therapy.
TBS delivers rapid bursts of magnetic pulses in a frequency pattern designed to mimic the brain’s natural rhythms. These sessions last only three minutes but offer comparable therapeutic outcomes to traditional TMS. By reducing treatment times, TBS improves patient compliance and makes TMS more accessible to individuals balancing therapy with other commitments.
Broader Applications of Magnetic Fields in Therapy
TMS has been studied and applied across a variety of conditions, demonstrating its broad potential. While this book will later delve deeply into specific applications, here are some of the key areas where TMS is making an impact:
- Anxiety Disorders: By targeting areas like the anterior cingulate cortex, TMS can help regulate fear and anxiety responses.
- Obsessive-Compulsive Disorder (OCD): Modulating hyperactive circuits in the prefrontal cortex can assist in reducing intrusive thoughts and compulsive behaviors.
- Smoking Cessation and Addiction: TMS has shown promise in disrupting neural pathways involved in cravings and reward-seeking behaviors.
- Post-Concussion Syndrome (PCS): For patients with lingering symptoms such as headaches, cognitive difficulties, and mood disruptions following a concussion, TMS offers a non-invasive option to restore neural balance.
- Chronic Pain: Stimulating the motor and somatosensory cortices helps to modulate pain perception, providing relief for conditions like fibromyalgia and neuropathic pain.
Looking Ahead
The science of magnetic fields in therapy forms the foundation for understanding TMS, but it is only the beginning. As TMS technology continues to evolve, it holds immense promise for expanding therapeutic applications. Future chapters will explore its role in neuroplasticity, imaging-guided targeting, and specific treatment protocols in greater detail.
Sources:
Pascual-Leone, A., et al. (2000). Transcranial magnetic stimulation in cognitive neuroscience. Current Opinion in Neurobiology, 10(2), 232-237. https://pubmed.ncbi.nlm.nih.gov/10753803/
Valero-Cabré, A., Amengual, J. L., et al. (2017). TMS in basic and clinical neuroscience. Neuroscientist, 23(4), 326-350. https://pubmed.ncbi.nlm.nih.gov/29032089/
Huang, Y. Z., et al. (2005). Theta burst stimulation of the human motor cortex. Neuron, 45(2), 201-206. https://doi.org/10.1016/j.neuron.2004.12.033
Barker, A. T., Jalinous, R., & Freeston, I. L. (1985). Non-invasive magnetic stimulation of the human motor cortex. The Lancet, 325(8437), 1106-1107. https://doi.org/10.1016/S0140-6736(85)92413-4



