TMS for Postpartum Depression: A Breakthrough Treatment for New Moms
Postpartum depression (PPD) is a serious mood disorder that affects many new mothers worldwide, with estimates suggesting that 1 in 7 women experiences symptoms after childbirth. Beyond the typical “baby blues,” postpartum depression can have long-lasting emotional, mental, and physical effects, impacting a mother’s well-being and her ability to bond with her newborn.
While traditional treatments like therapy and medication are often effective, some women continue to struggle with symptoms that affect daily life. Transcranial Magnetic Stimulation (TMS) is a cutting-edge, non-invasive treatment that has emerged as a promising option for mothers with PPD who need more than conventional therapy.
In this comprehensive guide, we’ll discuss what postpartum depression is, how TMS works, the benefits, what to expect during treatment, and why Palmier TMS is a trusted provider in Missouri.
Understanding Postpartum Depression
Postpartum depression (PPD) is more than typical “baby blues.” It is a serious medical condition that affects mothers after childbirth, impacting their ability to function, care for themselves, and bond with their baby. Symptoms vary in severity and can include persistent sadness, anxiety, irritability, fatigue, changes in appetite, sleep disturbances, feelings of guilt or worthlessness, and loss of interest in activities once enjoyed. PPD can appear anytime within the first year after delivery and may interfere with daily life and relationships. Early recognition, support from loved ones, and professional treatment are essential for recovery and well-being.
Common Symptoms of Postpartum Depression
- Persistent sadness, anxiety, or feelings of emptiness
- Mood swings and irritability
- Difficulty bonding with the baby
- Changes in sleep patterns or appetite
- Feelings of guilt, worthlessness, or hopelessness
- Loss of interest in previously enjoyable activities
- Physical symptoms such as fatigue or headaches
It’s important to differentiate PPD from the “baby blues,” which affect up to 80% of new mothers. Baby blues typically involve mood swings and tearfulness during the first two weeks postpartum and resolve without treatment. In contrast, postpartum depression persists longer, often intensifying over time if untreated.
Causes and Risk Factors
The exact cause of postpartum depression (PPD) is not fully understood, but it is believed to result from a combination of biological, psychological, and social factors. Hormonal changes after childbirth, such as shifts in estrogen and progesterone, can affect brain chemistry and mood regulation. Psychological factors, including a history of depression, anxiety, or stressful life events, can increase vulnerability. Social influences, such as lack of support from family or partners, financial stress, and major life changes, also play a role. Understanding that multiple factors contribute to PPD highlights the importance of comprehensive support, early detection, and professional intervention for affected mothers.
- Hormonal Changes: Rapid drops in estrogen and progesterone after delivery can affect brain chemistry.
- Previous Mental Health Issues: Women with a history of depression or anxiety are at higher risk.
- Stressful Life Events: Financial stress, lack of support, or relationship challenges can trigger PPD.
- Sleep Deprivation: Caring for a newborn often leads to chronic sleep loss, worsening mood symptoms.
Recognizing the signs early and seeking professional help is crucial for recovery.
Traditional Treatments for Postpartum Depression
Traditionally, postpartum depression (PPD) has been treated through a combination of therapy, medication, and lifestyle interventions. Psychotherapy, such as cognitive-behavioral therapy (CBT) or interpersonal therapy (IPT), helps mothers process emotions, develop coping strategies, and improve relationships. Medications, including certain antidepressants, can help regulate mood and reduce symptoms, especially when prescribed and monitored by healthcare professionals. Lifestyle interventions, such as regular exercise, proper nutrition, sufficient rest, and strong social support, also play a crucial role in recovery. Combining these approaches provides a holistic plan that addresses both the emotional and physical aspects of postpartum depression.
1. Therapy
Cognitive-Behavioral Therapy (CBT) and interpersonal therapy are common approaches. Therapy helps mothers:
- Identify and change negative thought patterns
- Develop coping strategies
- Improve communication and relationships
- Gain emotional support
While therapy is effective for many, some mothers may not respond fully or quickly enough to see improvement.
2. Medication
Antidepressants such as selective serotonin reuptake inhibitors (SSRIs) are sometimes prescribed. However:
- Some medications may not be suitable for breastfeeding mothers
- Side effects can include nausea, fatigue, or dizziness
- Medication alone may not fully address all symptoms
3. Lifestyle Interventions
Exercise, proper nutrition, adequate sleep, and support groups can enhance recovery but may not be sufficient for moderate to severe cases of PPD.
This gap in treatment options is where TMS therapy comes in—a non-invasive, effective alternative for mothers struggling with postpartum depression.
What is TMS Therapy?
Transcranial Magnetic Stimulation (TMS) is an FDA-approved, non-invasive treatment for depression, including postpartum depression. Unlike medications, TMS works by directly stimulating specific areas of the brain that regulate mood, using magnetic pulses. This targeted approach helps improve depressive symptoms without the systemic side effects commonly associated with drugs. TMS is typically administered in a series of outpatient sessions, allowing patients to continue daily activities during treatment. It is especially beneficial for those who have not responded well to traditional therapies or medications. Research shows TMS can effectively reduce symptoms and improve overall emotional well-being.
How TMS Works
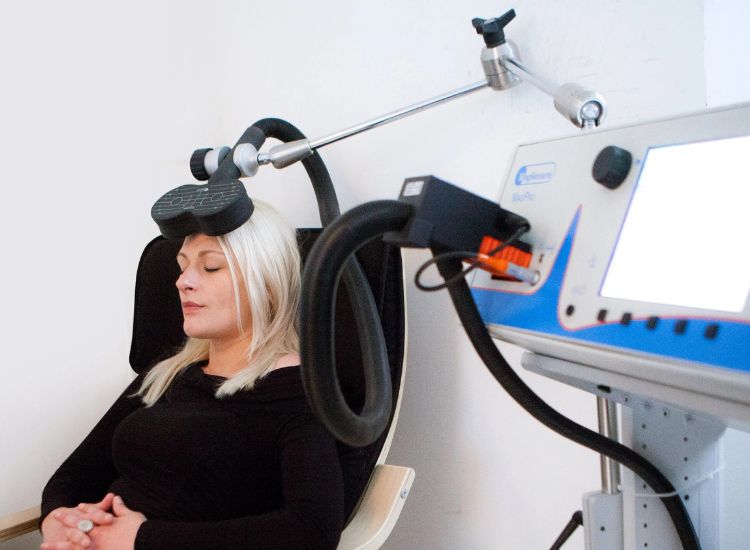
- Magnetic Pulses: A specialized electromagnetic coil is placed on the scalp, delivering focused magnetic pulses.
- Neuron Activation: The pulses stimulate nerve cells in the prefrontal cortex, an area associated with mood and emotion.
- Neurotransmitter Release: The stimulation encourages the release of serotonin, dopamine, and other mood-regulating chemicals.
- Gradual Improvement: Over multiple sessions, this enhanced brain activity reduces depressive symptoms and improves emotional resilience.
Unlike electroconvulsive therapy (ECT), TMS does not require anesthesia or induce seizures, making it a safer and more comfortable option for postpartum mothers.
Benefits of TMS for Postpartum Depression
TMS therapy offers several advantages, particularly for mothers looking for non-pharmacological treatments for postpartum depression. As a non-invasive procedure, it directly targets brain regions involved in mood regulation without affecting the rest of the body, minimizing side effects. Unlike medications, TMS does not interfere with breastfeeding, making it a safer option for new mothers. Treatments are performed on an outpatient basis, allowing mothers to maintain daily routines. TMS has shown effectiveness in reducing depressive symptoms, improving emotional stability, and enhancing quality of life. For mothers seeking safe, targeted, and drug-free solutions, TMS presents a promising alternative.
- Non-Invasive: No surgery, anesthesia, or systemic side effects.
- Safe for Breastfeeding: TMS does not affect breast milk or harm the baby.
- Effective: Many patients who did not respond to medication experience significant improvement.
- Minimal Side Effects: Mild scalp discomfort or headache are the most common, typically resolving quickly.
- Improved Quality of Life: TMS reduces depressive symptoms, enhances mood, and strengthens mother-infant bonding.
Research supports TMS as a promising therapy for women with treatment-resistant postpartum depression, offering hope when traditional methods fall short.
The TMS Treatment Process
Understanding what to expect from TMS therapy can help make the process less intimidating for new mothers. Sessions are typically conducted in a comfortable outpatient setting, lasting about 20–40 minutes each. During treatment, a magnetic coil is placed near the scalp to stimulate specific brain regions, producing mild tapping sensations but causing minimal discomfort. Patients remain fully awake and alert, allowing them to return to daily activities immediately afterward. Knowing the procedure is non-invasive, painless, and does not interfere with breastfeeding can reduce anxiety. Clear expectations and professional guidance help mothers feel confident and supported throughout TMS therapy.
Step 1: Consultation
At Palmier TMS, the process begins with a comprehensive evaluation. A provider will:
- Review your medical history and prior treatments
- Assess your PPD symptoms
- Determine if TMS is the right approach for your situation
Step 2: Personalized Treatment Plan
Each patient receives a customized plan, including:
- Number of sessions (typically 20–30)
- Frequency and duration of treatment (usually daily sessions, 5 days a week for 4–6 weeks)
- Targeted brain regions based on individual needs
Step 3: Treatment Sessions
During a session:
- The patient sits comfortably while a magnetic coil is placed on the scalp
- Pulses are delivered, stimulating brain activity
- Patients remain awake and alert, often reading or listening to music
Step 4: Monitoring and Adjustments
Providers monitor patient responses, adjusting intensity and placement as needed to maximize benefits.
Step 5: Ongoing Assessment
Progress is tracked throughout treatment. Many patients report symptom improvement within 2–4 weeks, with continued benefits after completing the full course.
Palmier TMS: Your Trusted Missouri Provider
Palmier TMS specializes in providing compassionate, effective care for mothers with postpartum depression. With three convenient locations across Missouri, they are committed to helping women regain their emotional well-being and enjoy their new role as mothers.
📍 Locations:
- Chesterfield: 112 Chesterfield Commons East Rd., Chesterfield, MO 63005
- Richmond Heights: 1505 S Big Bend Blvd, Richmond Heights, MO 63117
- Osage Beach (Ozarks): 5721 Osage Beach Parkway, Suite #300, Osage Beach, MO 65065
🌐 Official Website: https://palmiertms.com
📞 Phone Number (Call or Text): 314-697-4867
Palmier TMS combines advanced technology with individualized care plans to ensure the best outcomes for mothers struggling with postpartum depression.
FAQs About TMS for Postpartum Depression
Q1: Is TMS safe for breastfeeding mothers?
Yes. TMS is non-invasive, does not involve medication, and is safe during breastfeeding.
Q2: How long before I see results?
Many patients notice improvements in mood within 2–4 weeks, with continued progress throughout the treatment course.
Q3: Are there side effects?
Side effects are generally mild and may include temporary headache, scalp discomfort, or tingling sensations.
Q4: Can TMS replace therapy or medication?
TMS can be used alone or alongside therapy and medication. Your provider will tailor the approach to your needs.
Q5: How many sessions will I need?
Most patients benefit from 20–30 sessions over 4–6 weeks, though treatment plans are personalized.
Q6: Is TMS covered by insurance?
Many insurance plans cover TMS for depression. Palmier TMS can assist with insurance verification and approval.
Q7: Can I continue my daily activities during treatment?
Yes. TMS sessions are outpatient procedures, allowing patients to resume normal activities immediately after treatment.
Research and Evidence Supporting TMS for Postpartum Depression
Several clinical studies demonstrate the efficacy of TMS for postpartum depression:
- A 2020 study in The Journal of Affective Disorders found that TMS significantly reduced depressive symptoms in postpartum women unresponsive to medication.
- Research indicates that TMS can improve mood and cognitive function without adverse effects on breastfeeding.
- Long-term studies suggest sustained symptom relief for many patients months after completing treatment.
These findings highlight TMS as a viable and evidence-based option for mothers who need a more effective solution.
Combining TMS with Holistic Postpartum Care
While TMS is highly effective, combining it with holistic postpartum care can optimize recovery:
- Therapy: Counseling or support groups complement TMS by addressing emotional and cognitive aspects.
- Lifestyle: Adequate sleep, exercise, and nutrition strengthen overall mental health.
- Support System: Family and partner support helps mothers adhere to treatment and recover more quickly.
This integrated approach ensures that mothers receive both biological and emotional support during their recovery journey.
Conclusion
Postpartum depression can feel overwhelming, making everyday tasks and bonding with your baby challenging. The good news is that it is treatable, and TMS therapy offers a safe, non-invasive, and effective solution, especially for mothers who have not found relief through traditional treatments like therapy or medication. TMS works by directly targeting specific areas of the brain involved in mood regulation, helping to restore emotional balance, improve overall mood, and support a stronger mother-child connection.
At Palmier TMS, mothers receive personalized treatment plans tailored to their unique needs. Using advanced TMS technology, our team provides compassionate, professional care in a comfortable environment. With three convenient locations across Missouri, accessing treatment is easier than ever. Recovery is possible, and no mother has to face postpartum depression alone. With the right support, TMS therapy can help you regain joy, confidence, and the emotional energy needed to nurture both yourself and your baby.
If you or a loved one is experiencing postpartum depression, take the first step toward relief today:
📞 Call or Text: 314-697-4867
🌐 Visit: https://palmiertms.com
📍 Locations:
- Chesterfield, MO
- Richmond Heights, MO
- Osage Beach, MO
Don’t wait—reclaim your emotional well-being and enjoy the joys of motherhood with the help of TMS therapy at Palmier TMS.



