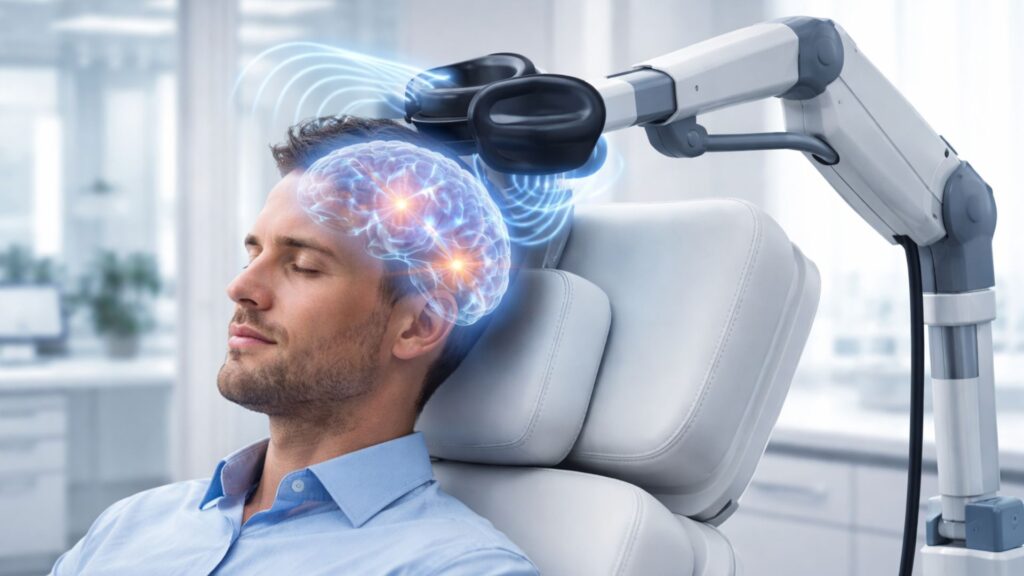
The Science Behind TMS: How Magnetic Pulses Help Rewire the Depressed Brain
Transcranial Magnetic Stimulation (TMS) has emerged as one of the most promising non-invasive treatments for depression, especially in individuals who haven’t found relief with traditional methods like medication and psychotherapy. Approved by the FDA, TMS offers a drug-free approach to managing depression by targeting specific areas of the brain that regulate mood—primarily the left dorsolateral prefrontal cortex.
TMS works by delivering magnetic pulses through a coil placed on the scalp. These pulses stimulate nerve cells in underactive regions of the brain associated with depression, helping to restore normal activity. Unlike antidepressants, which can take weeks to work and often come with side effects, TMS typically produces improvements within a few weeks and has minimal side effects—most commonly, mild scalp discomfort or headache.
One of the biggest advantages of TMS is its non-invasive nature. There’s no anesthesia, no need for recovery time, and patients can return to daily activities immediately after a session. As research continues to support its effectiveness, TMS is quickly gaining traction as a safe and effective alternative or supplement to conventional depression treatments. For many, it represents a hopeful step forward in achieving long-term relief and a better quality of life.
What is Transcranial Magnetic Stimulation (TMS)?
Transcranial Magnetic Stimulation (TMS) has emerged as one of the most promising non-invasive treatments for depression, especially in individuals who haven’t found relief with traditional methods like medication and psychotherapy. Approved by the FDA, TMS offers a drug-free approach to managing depression by targeting specific areas of the brain that regulate mood—primarily the left dorsolateral prefrontal cortex.
TMS works by delivering magnetic pulses through a coil placed on the scalp. These pulses stimulate nerve cells in underactive regions of the brain associated with depression, helping to restore normal activity. Unlike antidepressants, which can take weeks to work and often come with side effects, TMS typically produces improvements within a few weeks and has minimal side effects—most commonly, mild scalp discomfort or headache.
One of the biggest advantages of TMS is its non-invasive nature. There’s no anesthesia, no need for recovery time, and patients can return to daily activities immediately after a session. As research continues to support its effectiveness, TMS is quickly gaining traction as a safe and effective alternative or supplement to conventional depression treatments. For many, it represents a hopeful step forward in achieving long-term relief and a better quality of life.
The Basics of TMS Treatment
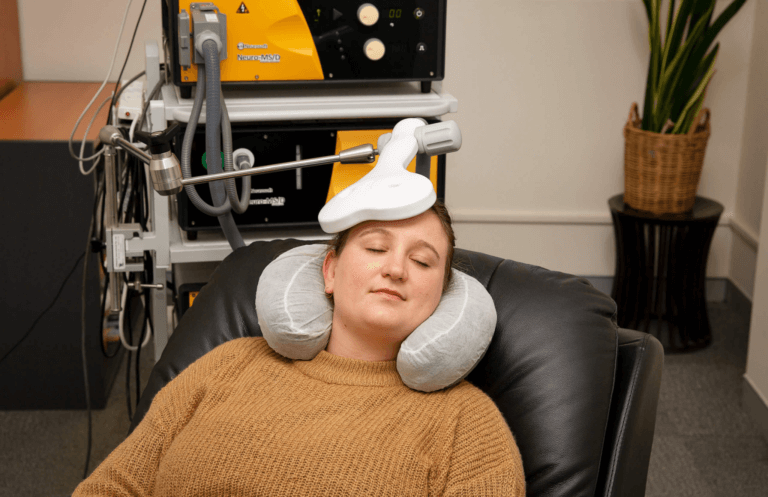
During a Transcranial Magnetic Stimulation (TMS) session, a specialized magnetic coil is positioned gently against the patient’s scalp, usually over the left prefrontal cortex—an area of the brain known to play a crucial role in mood regulation. Once the coil is in place, it delivers repetitive magnetic pulses that penetrate the skull and stimulate the targeted brain region. These pulses are completely non-invasive and painless, though some individuals may experience a mild tapping sensation or slight discomfort on the scalp during treatment.
Each pulse generates a brief magnetic field that induces small electrical currents in the brain tissue. These currents help activate underactive neurons and modulate the brain’s electrical activity, which is often disrupted in individuals with depression and other mood disorders. Over time, and through repeated sessions, this stimulation encourages healthier neural communication and improved emotional processing.
A typical TMS session lasts between 20 to 40 minutes, and patients can remain fully awake and alert throughout the procedure. There is no need for sedation or anesthesia, and most people can resume their normal daily activities immediately afterward. As treatments progress over several weeks, many patients begin to notice a significant reduction in depressive symptoms, offering hope and relief where other therapies may have failed.
How Does TMS Work to Treat Depression?

The underlying cause of depression is often linked to abnormal neural activity in the brain, particularly in regions responsible for mood regulation, decision-making, and emotional response. One key area that plays a central role is the left prefrontal cortex. In people with depression, this part of the brain is frequently underactive, contributing to symptoms such as persistent sadness, lack of motivation, poor concentration, and emotional numbness.
Transcranial Magnetic Stimulation (TMS) therapy addresses this issue by delivering focused magnetic pulses directly to the left prefrontal cortex. These pulses create small electrical currents that stimulate nerve cells, enhancing communication between different brain regions and helping to restore more balanced brain activity. Over time, this stimulation can lead to significant improvements in mood and overall emotional functioning.
Unlike medications that affect the brain chemically and can lead to widespread side effects, TMS is precise and non-invasive. This makes it a highly attractive option for individuals who have not responded to or cannot tolerate traditional antidepressants. By directly targeting the neural circuits involved in depression, TMS offers a promising, science-backed method for alleviating symptoms and helping patients regain control of their lives. As research continues to advance, TMS is reshaping how we understand and treat depression.
Magnetic Pulses and Neural Activity
TMS works by generating a focused magnetic field that induces small electrical currents within the brain. These currents specifically target the prefrontal cortex, an area often underactive in individuals with depression. By stimulating these neurons, TMS increases their activity, helping to restore normal brain function. The repetitive pulses delivered during each session are key to promoting neuroplasticity—the brain’s natural ability to adapt and form new neural pathways. Over time, this rewiring effect helps improve mood regulation and emotional response. This non-invasive approach makes TMS an effective option for patients who have not benefited from traditional antidepressant treatments.
Effect on Neurotransmitter Levels
Transcranial Magnetic Stimulation (TMS) is a non-invasive therapy that uses magnetic pulses to stimulate specific areas of the brain involved in mood regulation, such as the prefrontal cortex. It works by influencing the activity and production of key neurotransmitters like serotonin, dopamine, and norepinephrine—chemicals often imbalanced in individuals with depression. Unlike antidepressant medications, TMS directly targets the brain without affecting the rest of the body, minimizing side effects. Over multiple sessions, patients typically experience improved mood, increased energy, and better emotional well-being. TMS is a safe, well-tolerated option, especially for those who haven’t found relief with traditional depression treatments.
The Benefits of TMS Over Traditional Treatments
While traditional treatments for depression, such as antidepressant medications, help many individuals, they are not effective for everyone. Some patients experience little to no relief, while others struggle with side effects like weight gain, fatigue, insomnia, or emotional numbness, which can lead to discontinuation of treatment. Transcranial Magnetic Stimulation (TMS) offers a promising alternative. It is non-invasive, medication-free, and generally well-tolerated. TMS directly targets areas of the brain involved in mood regulation, providing symptom relief without the systemic side effects of drugs. For those who haven’t responded to medications, TMS can be a safe and effective path to recovery.
Non-invasive and Painless
Transcranial Magnetic Stimulation (TMS) is a non-invasive treatment that does not require surgery, implants, or anesthesia, making it a convenient and low-risk option for managing depression. Most patients experience little to no discomfort during the procedure, which involves sitting comfortably while magnetic pulses are delivered to targeted areas of the brain. Each session typically lasts between 20 to 40 minutes, depending on the individual’s treatment plan. One of the biggest advantages of TMS is that there is no downtime—patients can drive themselves to and from appointments and resume normal daily activities immediately after each session.
No Systemic Side Effects
Unlike antidepressant medications, which can cause a variety of side effects such as weight gain, fatigue, insomnia, or sexual dysfunction, Transcranial Magnetic Stimulation (TMS) is known for its minimal side effects. The most commonly reported side effect is mild scalp discomfort or a headache during or after treatment, which usually subsides after the first few sessions. TMS does not involve any sedation, medication, or invasive procedures, making it a well-tolerated option for most patients. With no systemic effects on the body, TMS offers a safer alternative for individuals seeking relief from depression without the burden of medication-related complications.
Faster Results with Long-Lasting Effects
While antidepressant medications can take weeks or months to show results, many patients begin to feel relief from TMS within a few sessions. Moreover, the effects of TMS can last for months or even years after the treatment ends, reducing the need for ongoing medication.
Who Can Benefit from TMS Treatment?
TMS is particularly beneficial for individuals who have:
- Major depressive disorder (MDD): Especially those who haven’t responded well to medications or therapy.
- Treatment-resistant depression: People who have tried multiple medications without finding relief.
- Anxiety, OCD, and PTSD: TMS has shown promise in treating these conditions as well, although it is not yet FDA-approved for them.
- Side effects from medications: TMS can be a viable option for those who experience intolerable side effects from antidepressants.
What to Expect During a TMS Session
Initial Consultation
Before starting TMS therapy, you will have a consultation with a TMS specialist who will assess your medical history and current condition. The specialist will determine if you are a good candidate for TMS.
The Procedure
- You will be asked to sit in a comfortable chair, and a magnetic coil will be placed on your scalp.
- The coil will generate magnetic pulses that target the brain’s prefrontal cortex. You may feel a tapping sensation on your head during the session, but it is generally not painful.
- Each session lasts around 20-40 minutes, and treatment typically occurs five days a week for 4-6 weeks.
Post-Treatment Care
There’s no downtime after a TMS session, and you can resume your normal activities immediately. Some patients may experience mild headaches or scalp discomfort, but these side effects usually dissipate quickly.
The Research Behind TMS: What Does the Science Say?
Studies have shown that TMS is an effective treatment for depression, with long-lasting effects. According to clinical trials and research conducted by the FDA, TMS has a success rate of about 50-60% for patients with treatment-resistant depression.
In addition to depression, TMS has been studied for other conditions, including anxiety, OCD, and even migraines. While more research is needed to establish its full range of benefits, the existing evidence is promising.
FAQs About TMS Treatment
Q: Is TMS FDA-approved?
Yes, TMS is FDA-approved for the treatment of major depressive disorder, especially in patients who have not responded to traditional medications.
Q: Is TMS covered by insurance?
Many insurance providers cover TMS treatment, especially when it’s prescribed for treatment-resistant depression. It’s best to check with your insurance provider to confirm coverage.
Q: How many TMS sessions will I need?
Most patients undergo 20-30 sessions over the course of 4-6 weeks. The number of sessions depends on the severity of your condition and your individual response to treatment.
Q: Does TMS have any side effects?
The most common side effects are mild headaches, scalp discomfort, and facial twitching during the session. These side effects are usually temporary and subside after treatment.
Q: Is TMS effective for everyone?
TMS is highly effective for many patients, but it doesn’t work for everyone. If you haven’t found relief from other treatments, TMS may be worth considering as a viable option.
Conclusion
Transcranial Magnetic Stimulation (TMS) is a revolutionary treatment that offers hope for people suffering from depression, especially those who haven’t found success with traditional therapies. By using magnetic pulses to stimulate the brain and restore neural activity, TMS helps rewire the brain and bring lasting relief to patients.
If you or someone you know is struggling with depression and other mental health conditions, TMS might be the breakthrough treatment you’ve been searching for.
Struggling with depression that won’t respond to medication? Discover how Transcranial Magnetic Stimulation (TMS) uses targeted magnetic pulses to safely and effectively rewire brain activity—offering real relief without side effects.
📍Visit us: 112 Chesterfield Commons East Rd, Chesterfield, MO 63005
📞Call: (314) 697-4867
📩Email: info@palmiertms.com
🌐Learn more or book a consultation at palmiertms.com
Sources
- FDA Approval of TMS for Depression
U.S. Food and Drug Administration. (2008). FDA approves neurostar TMS system for treatment of major depression. FDA.gov - Efficacy of TMS in Treatment-Resistant Depression
O’Reardon, J. P., Solvason, H. B., Janicak, P. G., et al. (2007). Efficacy and safety of transcranial magnetic stimulation in the acute treatment of major depression: a multisite randomized controlled trial. Biological Psychiatry, 62(11), 1208-1216.
https://doi.org/10.1016/j.biopsych.2007.01.018 - Mechanism of Action of TMS
George, M. S., & Post, R. M. (2011). Daily left prefrontal repetitive transcranial magnetic stimulation for acute treatment of medication-resistant depression. American Journal of Psychiatry, 168(4), 356-364.
https://doi.org/10.1176/appi.ajp.2010.10040500 - TMS and Neurotransmitters
Baeken, C., & De Raedt, R. (2013). The neurobiological mechanisms of repetitive transcranial magnetic stimulation in depression. Neuroscience & Biobehavioral Reviews, 37(9), 2440-2452.
https://doi.org/10.1016/j.neubiorev.2013.06.003 - Safety and Side Effects of TMS
Lefaucheur, J. P., André-Obadia, N., Antal, A., et al. (2014). Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS). Clinical Neurophysiology, 125(11), 2150-2206.
https://doi.org/10.1016/j.clinph.2014.05.021 - Insurance Coverage for TMS
National Alliance on Mental Illness (NAMI). Insurance Coverage for TMS. NAMI.org - TMS in Anxiety and OCD
Dunlop, K., & Mayberg, H. (2014). Neuroimaging and Neuromodulation in Treatment-Resistant Depression and OCD. Biological Psychiatry, 75(3), 187-193.
https://doi.org/10.1016/j.biopsych.2013.08.011