The Link Between Mental Health and Chronic Pain: How TMS Offers Relief
Chronic pain is a debilitating condition that affects millions globally, often extending far beyond physical discomfort. It can disrupt sleep, impair daily functioning, strain personal relationships, and lead to significant emotional distress. The link between chronic pain and mental health is profound, with many individuals experiencing depression, anxiety, or both as a result of their ongoing suffering. This bidirectional relationship means that chronic pain can worsen mental health, and poor mental health can amplify the perception of pain. Over time, chronic pain may alter brain function, particularly in areas responsible for mood regulation, pain perception, and emotional processing. Traditional treatments—such as pain medications, physical therapy, and psychotherapy—often provide limited relief, especially when pain and mental health issues occur together. As a result, many patients are left searching for more comprehensive, effective options. One such emerging treatment is Transcranial Magnetic Stimulation (TMS). TMS is a non-invasive, FDA-approved procedure that uses magnetic fields to stimulate specific areas of the brain involved in mood regulation and pain perception. It has shown promise not only in treating depression and anxiety but also in alleviating certain types of chronic pain. Studies suggest that TMS can help “reset” neural pathways, improve emotional resilience, and reduce pain intensity. For individuals with treatment-resistant depression and chronic pain, TMS offers hope without the side effects associated with medications. A typical TMS session lasts 20–40 minutes, is done five days a week over several weeks, and requires no anesthesia or recovery time. Patients often report feeling more emotionally balanced and physically comfortable after a few sessions. In conclusion, TMS represents a promising solution for those struggling with the complex intersection of chronic pain and mental health. If you’re exploring options beyond traditional treatments, consult a TMS specialist to determine if this innovative therapy is right for you.
Understanding the Connection Between Chronic Pain and Mental Health
Chronic pain, defined as pain that persists for longer than three to six months, can have profound effects not only on the body but also on an individual’s emotional and psychological well-being. Unlike acute pain, which serves a biological purpose by signaling injury and promoting healing, chronic pain often continues long after the original injury has healed—or may even arise without a clear cause. This ongoing discomfort can severely disrupt a person’s quality of life, leading to a range of emotional challenges. Many individuals living with chronic pain experience depression, anxiety, and sleep disturbances. The continuous nature of the pain can cause irritability and frequent mood swings, making it difficult to maintain stable relationships and engage in everyday activities. Social withdrawal is also common, as people may isolate themselves due to the unpredictability of their pain or feelings of being misunderstood by others. Research shows that up to 85% of people with chronic pain also suffer from severe depression, highlighting the deep emotional toll it can take. This relationship is bidirectional—meaning mental health issues like anxiety and depression can worsen the perception of pain, while the unrelenting experience of pain can, in turn, intensify emotional distress. Over time, this vicious cycle can become difficult to break without comprehensive treatment that addresses both the physical and emotional aspects of chronic pain. Effective management often involves a multidisciplinary approach, including medication, physical therapy, psychological counseling, and lifestyle changes. Recognizing the emotional burden of chronic pain is crucial, as treating the mind is just as important as treating the body. Support systems, professional help, and increased awareness can make a significant difference in improving the quality of life for those who live with chronic pain on a daily basis.
How Chronic Pain Affects the Brain
Chronic pain is far more than just a physical sensation—it fundamentally alters the way the brain functions, reshaping emotional and cognitive responses over time. When pain becomes persistent, it continuously activates the nervous system, sending signals that stimulate key areas of the brain responsible for emotion, decision-making, and memory. The prefrontal cortex, which governs mood regulation and decision-making, becomes overstimulated, often leading to impaired cognitive function and increased feelings of anxiety or depression. Similarly, the anterior cingulate cortex, a region involved in processing both physical pain and emotional distress, becomes more sensitive, making individuals not only more aware of their pain but also more emotionally reactive to it. The amygdala, the brain’s center for emotional processing and fear response, also becomes hyperactive, reinforcing feelings of stress, fear, and helplessness. These neurological changes don’t just occur as a response to chronic pain—they become part of the brain’s new baseline function, essentially rewiring it. Over time, this neuroplasticity contributes to a heightened sensitivity to pain and a lower threshold for emotional regulation. This shift can pave the way for the development or worsening of mental health disorders such as depression and anxiety. As depression deepens, it can further distort pain perception, creating a self-perpetuating cycle where emotional suffering amplifies physical pain, and vice versa. This vicious loop significantly impacts quality of life, as sufferers become trapped in an ongoing feedback system of physical and emotional distress. Effective treatment, therefore, must address not only the physical component of chronic pain but also the emotional and neurological changes that accompany it. Understanding this complex interaction between chronic pain and the brain is essential for developing integrated, long-term solutions that improve both physical and mental well-being.
The Limitations of Conventional Treatments
For years, chronic pain has been treated with a mix of medications, physical therapy, and lifestyle changes. While these can offer temporary relief, they often fall short in addressing the psychological components of chronic pain.
Common Limitations:
- Pain medications (such as opioids) can lead to dependence and don’t address the emotional root causes.
- Antidepressants might relieve mood symptoms but often come with side effects or limited efficacy.
- Talk therapy is beneficial but may not be enough for treatment-resistant depression.
- Surgical options may not always be suitable or effective, especially if the source of pain is unclear.
So, what happens when traditional treatments don’t work? This is where Transcranial Magnetic Stimulation (TMS) comes in.
What is TMS?
Transcranial Magnetic Stimulation (TMS) is a non-invasive, FDA-cleared therapy that uses magnetic pulses to stimulate the left dorsolateral prefrontal cortex—an area of the brain often underactive in individuals suffering from depression and chronic pain. By targeting this specific region, TMS helps to improve brain function, reduce the perception of pain, and alleviate symptoms of depression and anxiety. Unlike traditional medications that introduce chemicals into the brain, TMS works by rewiring neural pathways, offering a drug-free and side-effect-free alternative for individuals who have not experienced relief through other treatments.
How TMS Helps Relieve Chronic Pain and Improve Mental Health
TMS was originally developed to treat major depressive disorder (MDD), especially in patients who haven’t responded to antidepressants. Over time, researchers discovered that TMS also significantly helps those suffering from chronic pain syndromes, including:
- Fibromyalgia
- Neuropathic pain
- Migraines
- Complex regional pain syndrome (CRPS)
- Back and neck pain
Mechanisms Behind TMS for Pain and Mood Relief:
- Neuroplasticity: TMS promotes the brain’s ability to reorganize and form new connections, especially in areas involved in both pain and mood.
- Endorphin Release: TMS stimulates the release of natural painkillers (endorphins) in the brain.
- Anti-inflammatory Effects: Chronic pain often causes inflammation in the brain. TMS helps reduce this inflammation.
- Enhanced Pain Tolerance: By altering the way pain signals are processed, TMS can increase a patient’s pain threshold.
Real Results from Real People
Many patients report not only a decrease in physical pain after TMS treatment but also a profound improvement in mood, energy, and overall quality of life.
“After years of living with both depression and back pain, TMS gave me back my life. I’m more active, more social, and the pain that ruled my life is now manageable.” — TMS patient testimonial
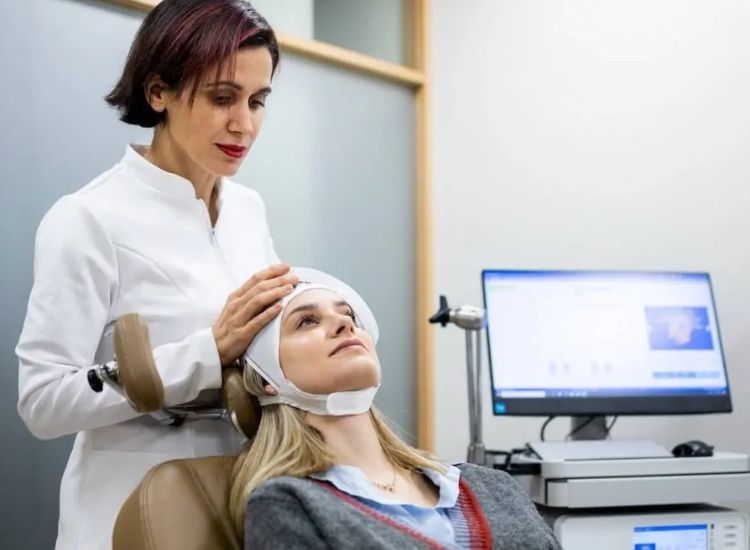
What to Expect During TMS Treatment
Each TMS session is quick and painless, lasting about 20–40 minutes. Here’s a breakdown of what happens:
- Initial Consultation: A trained TMS provider will evaluate your symptoms and medical history to determine if TMS is right for you.
- Mapping Session: During your first appointment, your doctor will locate the exact area of the brain to target using specialized mapping techniques.
- Treatment Sessions: You’ll visit the clinic five days a week for about 6–8 weeks. Many patients begin noticing improvement within 2–3 weeks.
- No Downtime: You can drive yourself to and from appointments, and return to daily activities immediately.
Is It Safe?
Transcranial Magnetic Stimulation (TMS) is a non-invasive, FDA-cleared treatment for depression and other mental health conditions. With over 15 years of clinical use and research, TMS has established itself as a safe and effective option for individuals who have not found relief through traditional treatments like medication or therapy. It works by delivering focused magnetic pulses to specific areas of the brain associated with mood regulation, stimulating neural activity and helping restore healthy brain function.
One of the most appealing aspects of TMS is its strong safety profile. Unlike medications, TMS does not circulate through the bloodstream, so it avoids many of the systemic side effects commonly associated with antidepressants, such as weight gain, sexual dysfunction, or fatigue. The most commonly reported side effects are minimal, including mild scalp discomfort or a headache at the treatment site. These side effects typically diminish after the first few sessions as the body adjusts to the stimulation. In rare cases, patients may experience lightheadedness or tingling in the facial muscles, but these symptoms are usually short-lived and well-tolerated.
A typical TMS treatment plan consists of five sessions per week over the course of four to six weeks, with each session lasting around 20 to 40 minutes. Patients remain awake and alert throughout the procedure and can resume normal activities immediately afterward, making TMS an excellent option for those with busy lifestyles.
Backed by extensive research and real-world success, TMS has shown positive outcomes for a wide range of patients. Clinical studies continue to demonstrate improvements in mood, concentration, and overall quality of life, even for individuals with treatment-resistant depression. As more patients and providers recognize the benefits of TMS, it is increasingly becoming a cornerstone of modern mental health care, offering hope and healing for those who need it most.
FAQs About TMS for Chronic Pain and Mental Health
Q: Is TMS painful?
A: No. Most patients describe the sensation as a light tapping or clicking sound. It’s non-invasive and doesn’t require anesthesia.
Q: How long does it take to see results?
A: Some people feel better after the first two weeks. Full results typically occur after 4–6 weeks of consistent treatment.
Q: Will insurance cover TMS?
A: Many insurance plans cover TMS for treatment-resistant depression. Coverage for pain-related treatment varies, so it’s best to contact us for a benefits check.
Q: Can TMS be used with other treatments?
A: Yes. TMS can be used alongside therapy, medications, and other pain management strategies.
Q: Who is NOT a candidate for TMS?
A: People with implanted metal or electronic devices near the head (like cochlear implants or pacemakers) may not be eligible. A full consultation is required to determine candidacy.
Conclusion
The connection between mental health and chronic pain is undeniable. When both conditions coexist, they can form a debilitating cycle that impacts every aspect of a person’s life. Traditional treatments often fall short, but TMS offers a new path forward—one that is safe, effective, and supported by science.
Chronic pain often leads to feelings of helplessness, frustration, and despair. Over time, this can evolve into clinical depression or anxiety disorders, making the experience of pain even more intense and difficult to manage. Mental health struggles can lower an individual’s pain threshold, disrupt sleep, and impair coping mechanisms, creating a vicious loop where both conditions feed into each other.
Transcranial Magnetic Stimulation (TMS) offers a breakthrough approach that addresses the neurological root of this cycle. Unlike medications that may only mask symptoms or come with a range of side effects, TMS works by stimulating specific areas of the brain involved in mood regulation and pain perception. It is non-invasive, FDA-approved, and has shown remarkable success in treating depression and certain types of chronic pain, particularly when other interventions have failed.
Patients undergoing TMS often report not only improved mood and mental clarity but also a noticeable reduction in their physical pain. As mental wellness improves, many find it easier to engage in physical therapy, sleep better, and regain a sense of control over their lives.
If you or a loved one are battling chronic pain and mental health challenges, know that relief is possible. You are not alone, and there are innovative treatments available. TMS can offer renewed hope and a brighter, pain-managed future—free from the overwhelming burden of two interlinked conditions. Reach out to learn more about how TMS might be the turning point you’ve been waiting for.
Start Your Healing Journey Today
If chronic pain and depression have been holding you back, it’s time to take action. At Palmier TMS Clinics, we specialize in compassionate, personalized care using the most advanced TMS technology available.
📞 Call us today at 314-697-4867 to schedule your free consultation and insurance verification.
You can visit us at any of our convenient Missouri locations:
CHESTERFIELD
📍 112 Chesterfield Commons East Rd.
Chesterfield, MO 63005
RICHMOND HEIGHTS
📍 1505 S Big Bend Blvd
Richmond Heights, MO 63117
OSAGE BEACH (OZARKS)
📍 5721 Osage Beach Parkway Suite #300
Osage Beach, MO 65065
👉 Learn more and request an appointment athttps://palmiertms.com/



