How TMS Works on the Brain Part 1:The Basics of Brain Stimulation with TMS
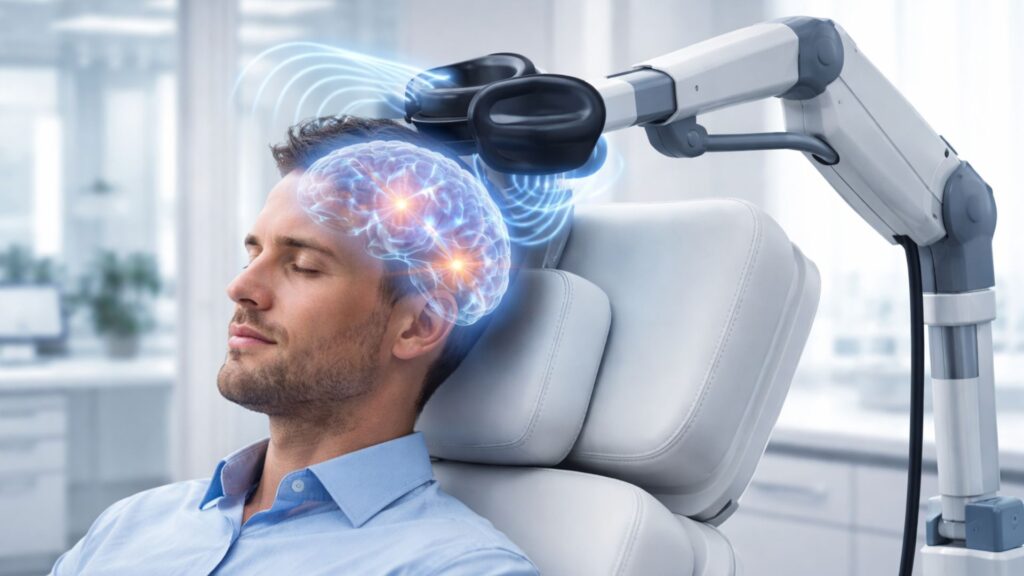
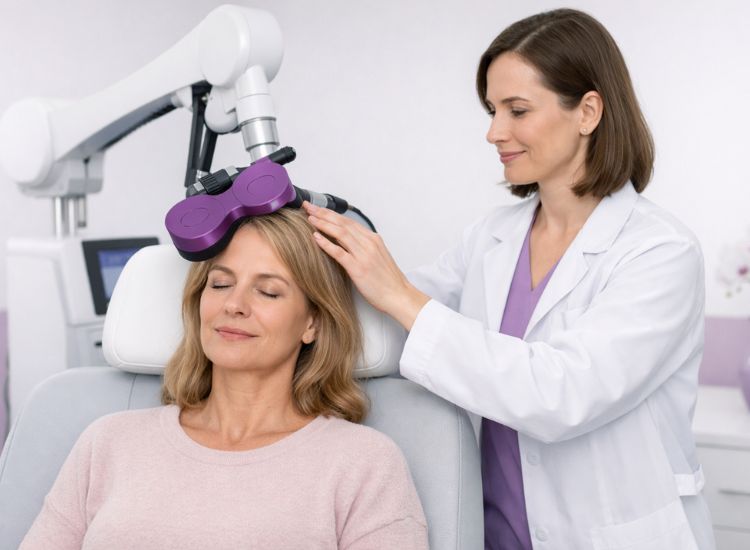
Transcranial Magnetic Stimulation (TMS) is a non-invasive neurostimulation technique that uses magnetic fields to induce electrical currents in targeted areas of the brain. This process has been instrumental in treating neurological and psychiatric disorders, especially major depressive disorder (MDD) and other conditions resistant to conventional therapies. Understanding the fundamental principles behind TMS provides insight into its mechanisms, benefits, and future potential.
TMS operates on the principle of electromagnetic induction, where a coil placed over the scalp generates a rapidly changing magnetic field. This magnetic field penetrates the skull and induces an electric current in the underlying neurons, causing them to depolarize and fire action potentials. This ability to directly influence neuronal activity allows TMS to modulate brain function, either increasing or decreasing activity depending on the stimulation parameters used. The intensity, duration, and frequency of stimulation determine whether the effect is excitatory or inhibitory.
One of the key distinguishing factors of TMS is its adaptability in terms of stimulation patterns. Single-pulse TMS is often used for research and diagnostics, mapping the brain’s responsiveness in specific regions. Paired-pulse TMS helps assess cortical excitability by delivering two pulses in succession, measuring how neurons respond. For therapeutic applications, repetitive TMS (rTMS) is used to deliver a series of pulses over time, inducing long-term effects in the brain’s neural networks. More recently, theta burst stimulation (TBS) has emerged as an accelerated method of stimulation, leveraging natural brain rhythms for a more efficient response.
TMS can produce both excitatory and inhibitory effects on neural circuits depending on the frequency used. High-frequency stimulation (≥5Hz) is typically associated with increased cortical excitability, frequently applied to the left dorsolateral prefrontal cortex (DLPFC) for the treatment of depression. Conversely, low-frequency stimulation (≤1Hz) reduces cortical excitability, which is beneficial in conditions such as anxiety, PTSD, and tinnitus. Theta Burst Stimulation (TBS) offers a condensed version of rTMS, with intermittent TBS (iTBS) acting similarly to high-frequency TMS and continuous TBS (cTBS) mimicking the effects of low-frequency TMS. The efficiency of iTBS has led to its FDA approval as a faster alternative to conventional TMS protocols for depression, significantly reducing session times while maintaining efficacy.
The impact of TMS is not limited to immediate neuronal activation; it also drives long-term neuroplastic changes. Short-term effects of TMS include temporary alterations in neuronal firing patterns, while long-term effects stem from sustained stimulation that strengthens or weakens neural connections. This neuroplasticity underlies the success of TMS in treating mental health disorders, allowing for structural and functional changes that extend beyond the duration of treatment. Studies indicate that repeated TMS sessions can lead to measurable improvements in brain function, reinforcing the concept that stimulation fosters adaptability within neural networks.
Despite its effectiveness, TMS remains a carefully regulated therapy with established safety protocols. The most common side effects include mild scalp discomfort, headaches, and facial muscle twitching during stimulation. The risk of seizures is extremely low, estimated at approximately one in 80,000 sessions. However, individuals with metal implants in the head, epilepsy, or certain neurological conditions require thorough screening to ensure the treatment is appropriate for them.
Looking ahead, advancements in TMS are shaping the future of neuromodulation. AI-driven TMS protocols are being developed to tailor stimulation settings based on individual brain activity patterns, improving precision and response rates. Wearable TMS devices are also in early development, offering the potential for at-home treatment options in the future. Furthermore, combination therapies integrating TMS with cognitive behavioral therapy (CBT) or pharmacological adjustments are being explored to enhance treatment outcomes.
TMS represents a significant advancement in neuropsychiatric treatment, offering a non-invasive method to modulate brain activity. Through various protocols, it can either excite or inhibit targeted brain regions, leading to therapeutic benefits for conditions such as depression, anxiety, and neurological disorders. As research progresses, personalized, AI-optimized, and home-based TMS treatments may revolutionize the field, making neuromodulation more precise and widely accessible.
References
- Blumberger, D. M., Vila-Rodriguez, F., Thorpe, K. E., Daskalakis, Z. J., & Downar, J. (2018). Effectiveness of theta burst versus high-frequency repetitive transcranial magnetic stimulation in patients with depression (THREE-D): A randomised non-inferiority trial. The Lancet, 391(10131), 1683-1692. https://doi.org/10.1016/S0140-6736(18)30295-2
- Lefaucheur, J. P., Aleman, A., Baeken, C., Benninger, D. H., Brunelin, J., Di Lazzaro, V., … & Ziemann, U. (2020). Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS). Clinical Neurophysiology, 131(2), 474-528. https://doi.org/10.1016/j.clinph.2019.11.002
- Chen, R., Classen, J., Gerloff, C., Celnik, P., Wassermann, E. M., Hallett, M., & Cohen, L. G. (1997). Depression of motor cortex excitability by low-frequency transcranial magnetic stimulation. Neurology, 48(5), 1398–1403. https://doi.org/10.1212/wnl.48.5.1398
- Cash, R. F. H., Weigand, A., Zalesky, A., Siddiqi, S. H., Downar, J., Fitzgerald, P. B., & Fox, M. D. (2021). Using Brain Imaging to Improve Spatial Targeting of Transcranial Magnetic Stimulation for Depression. Biological psychiatry, 90(10), 689–700. https://doi.org/10.1016/j.biopsych.2020.05.033