How TMS Works on the Brain Part 2:Electrical Currents Induced by Magnetic Fields
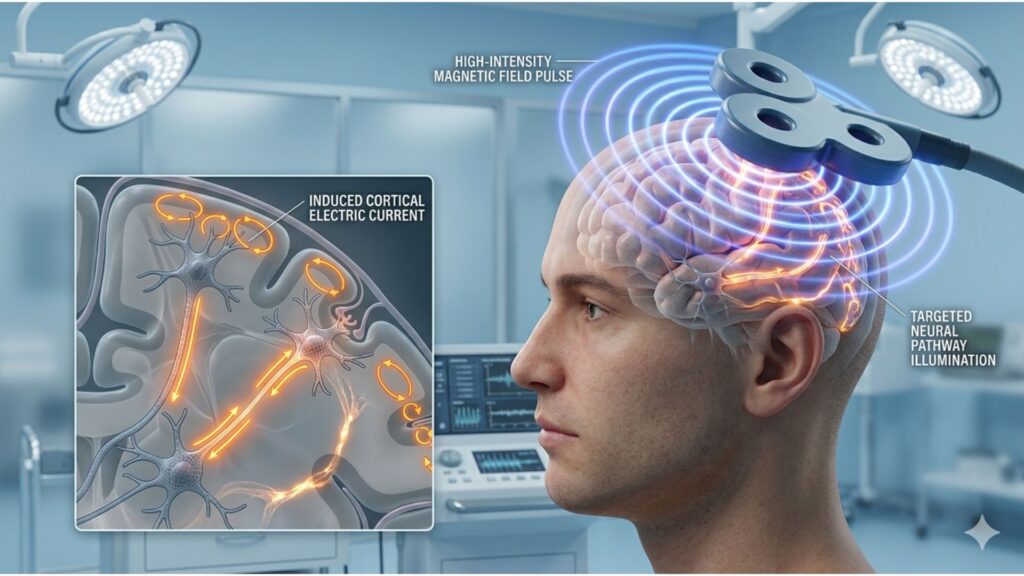
Transcranial Magnetic Stimulation (TMS) operates on the principle of electromagnetic induction, a phenomenon first described by Michael Faraday in 1831. By using rapidly changing magnetic fields, TMS generates electrical currents in targeted brain regions, modulating neural activity in a controlled and non-invasive manner. Understanding how these electrical currents are induced and their effects on brain physiology is key to grasping the mechanism behind TMS’s therapeutic impact.
The Physics of Electromagnetic Induction in TMS
TMS works by delivering a pulsed magnetic field via a coil placed on the scalp. The rapidly fluctuating magnetic field penetrates the skull without resistance and induces an electric current in the underlying neurons. This process follows Faraday’s Law of Electromagnetic Induction, which states that a changing magnetic field creates an electric field in a conductor—in this case, brain tissue.
The induced electric current affects neurons by modulating their membrane potential, either depolarizing or hyperpolarizing them, depending on the stimulation parameters. This leads to action potentials in excitable cells, altering neural firing patterns and influencing brain network connectivity. The strongest currents are typically generated in superficial cortical layers (1-3 cm beneath the skull), with coil placement determining the precise focal point of stimulation.
How TMS-Induced Electrical Currents Affect Neurons
When a TMS pulse reaches the brain, it interacts with neurons in multiple ways. Primarily, it stimulates long-range pyramidal neurons and interneurons, which influences network activity beyond the immediate stimulation site. The depolarization of neurons also triggers neurotransmitter release, including dopamine, serotonin, and glutamate, which play key roles in mood regulation, cognitive function, and motor control.
This electrical activity can lead to two primary effects:
- Excitation: High-frequency TMS (≥5Hz) increases cortical excitability, commonly used to enhance brain function in depression treatment.
- Inhibition: Low-frequency TMS (≤1Hz) suppresses activity in hyperactive regions, often applied in conditions like anxiety, PTSD, and tinnitus.
A more recent innovation, Theta Burst Stimulation (TBS), delivers short bursts of pulses that mimic natural brain rhythms. This method enhances long-term synaptic changes, contributing to sustained therapeutic effects.
Key Factors Influencing Current Distribution
The distribution and depth of the induced electrical currents depend on several factors. Coil design plays a major role in determining stimulation accuracy. For instance, a figure-eight coil provides highly focused stimulation, making it ideal for precise targeting of cortical areas, whereas an H-coil, used in deep TMS (dTMS), reaches deeper brain structures like the anterior cingulate cortex and insula.
Beyond coil shape, pulse frequency and duration impact whether TMS stimulates or suppresses activity. High-frequency pulses enhance synaptic plasticity, whereas lower frequencies create inhibitory effects. Additionally, individual brain anatomy influences the extent of current penetration. MRI-guided neuronavigation is now widely used to optimize coil placement, ensuring that stimulation is accurately delivered to the intended brain region.
Therapeutic Applications of TMS-Induced Electrical Currents
TMS’s ability to modulate neural circuits through electrical currents has led to its application in various disorders. In major depressive disorder (MDD), stimulation of the left dorsolateral prefrontal cortex (DLPFC) enhances its connectivity with the limbic system, helping counteract hypoactivity in emotional regulation circuits. For obsessive-compulsive disorder (OCD), targeting the anterior cingulate cortex reduces compulsive thought patterns by modulating dysfunctional brain loops.
The technology is also being explored in chronic pain management, where TMS applied to the primary motor cortex (M1) alters pain-processing pathways. Similarly, in stroke rehabilitation, stimulation of perilesional areas facilitates neuronal reorganization, promoting recovery of motor function.
Advancements in Electrical Current Modeling for TMS
With the integration of computational modeling and imaging technology, researchers have significantly improved precision in targeting specific brain regions. Finite Element Modeling (FEM) predicts the depth and distribution of induced currents, while neuronavigation-guided TMS uses real-time imaging to dynamically adjust stimulation settings for each individual. These innovations allow for personalized treatment approaches, increasing TMS’s effectiveness across different patient populations.
Conclusion
TMS-induced electrical currents are at the core of its ability to modulate neural circuits and drive therapeutic benefits. By understanding how electromagnetic induction interacts with brain tissue, clinicians can optimize TMS protocols to treat a range of psychiatric and neurological disorders. As neuronavigation, AI-driven stimulation, and individualized treatment plans continue to evolve, TMS is poised to become an even more precise and impactful tool in reshaping brain function.
References
- Sun, W., Wu, Q., Gao, L., Zheng, Z., Xiang, H., Yang, K., Yu, B., & Yao, J. (2023). Advancements in Transcranial Magnetic Stimulation Research and the Path to Precision. Neuropsychiatric disease and treatment, 19, 1841–1851. https://doi.org/10.2147/NDT.S414782
- Cash, R. F. H., Weigand, A., Zalesky, A., Siddiqi, S. H., Downar, J., Fitzgerald, P. B., & Fox, M. D. (2021). Using Brain Imaging to Improve Spatial Targeting of Transcranial Magnetic Stimulation for Depression. Biological psychiatry, 90(10), 689–700. https://doi.org/10.1016/j.biopsych.2020.05.033
- Lefaucheur, J. P., Aleman, A., Baeken, C., Benninger, D. H., Brunelin, J., & Di Lazzaro, V. (2020). Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS). Clinical Neurophysiology, 131(2), 474-528. https://doi.org/10.1016/j.clinph.2019.11.002
- Chen, Mo, Cline, Christopher C., et al. (2019). Advances and Challenges in Transcranial Magnetic Stimulation (TMS) Research on Motor Systems. Engineering in Medicine. 283-318. https://www.sciencedirect.com/science/article/abs/pii/B9780128130681000117