A Day in TMS Therapy: What to Expect from Evaluation to Daily Sessions
For many people living with major depressive disorder or other mood disorders, finding relief can be a long and frustrating journey. Traditional treatments — like antidepressant medications and talk therapy — can be effective, but not for everyone. In fact, research shows that more than one-third of patients may not achieve full remission with medication alone.
This is where Transcranial Magnetic Stimulation (TMS) offers a promising alternative.
At Palmier TMS & Behavioral Health, we’ve helped patients who felt they had exhausted every option. TMS is a safe, non-invasive treatment that uses magnetic pulses to stimulate specific areas of the brain linked to mood regulation. For many, it has led to significant improvement in symptoms — even after years of struggle.
We understand that starting a new treatment can feel overwhelming, especially one involving advanced technology, brain stimulation, and multiple weekly clinic visits. That’s why we’re committed to making your experience as comfortable and transparent as possible.
In this article, we’ll walk you through what to expect — from your first evaluation to what daily sessions look like — so you can feel informed, confident, and ready to take the next step toward hope and healing with TMS.
What Is TMS Therapy and How Does It Work?
Transcranial Magnetic Stimulation (TMS) is an FDA-cleared, non-invasive brain stimulation therapy designed to treat depression and certain other mental health conditions. Unlike medications, which affect the entire body, TMS targets specific areas of the brain involved in mood regulation — most notably the left dorsolateral prefrontal cortex (DLPFC). This region plays a key role in controlling emotions, decision-making, and stress responses.
During a TMS session, a specialized device delivers gentle, focused magnetic pulses to this targeted brain area. These pulses pass painlessly through the scalp and skull, activating underactive nerve cells. By stimulating these neurons, TMS helps improve communication between different brain regions, restoring more balanced brain activity. Over time, this can promote healthier mood patterns and reduce symptoms of depression.
TMS is especially valuable for individuals who haven’t experienced sufficient relief from antidepressant medications or who cannot tolerate their side effects. Because it’s non-invasive, there is no surgery, anesthesia, or recovery time required. Most patients can return to their normal activities immediately after each session.
With consistent treatment, many people notice gradual improvements in mood, energy levels, and overall quality of life — making TMS a hopeful option for those seeking a new path toward mental wellness.
Key points to know about TMS:
- Non-invasive: No surgery, anesthesia, or sedation is involved.
- Safe & well-tolerated: Most patients experience little to no significant side effects.
- No downtime: You can immediately return to work, school, or errands after treatment.
- Personalized: We tailor the treatment intensity and target location to your unique brain activity.
Step One: The Comprehensive Evaluation
Before beginning Transcranial Magnetic Stimulation (TMS) therapy, we conduct a comprehensive evaluation to ensure it’s the right treatment for you. This first step is important because TMS, while highly effective for many, works best when it’s carefully matched to the patient’s individual needs and medical history.
During your evaluation, one of our experienced providers will take time to understand your symptoms, mental health history, and previous treatments. We’ll ask about your experiences with medications, therapy, and any other approaches you’ve tried, as well as how your depression or mood disorder affects your daily life. We also review your overall health, including any neurological conditions, medications you’re currently taking, or factors that might influence treatment.
In some cases, additional assessments — such as questionnaires or depression rating scales — may be used to measure your baseline mood and track progress over time. This thorough process not only helps confirm that TMS is a safe and suitable option, but also allows us to tailor your treatment for maximum benefit.
By the end of your evaluation, you’ll have a clear understanding of how TMS works, what to expect, and the personalized plan we’ve designed to help you move toward lasting relief and improved well-being.
What We Cover During the Evaluation
- Medical and Psychiatric History
We review your diagnosis, symptoms, and previous treatment history. This includes any medications you’ve tried, psychotherapy experiences, and whether you’ve had any hospitalizations for mental health. - Current Symptoms
We talk about your daily mood patterns, energy levels, sleep habits, and motivation. You may also complete standardized questionnaires that help us track your progress throughout the treatment. - Physical Safety Screening
Because TMS uses magnetic fields, patients with certain implanted devices (like deep brain stimulators or metallic fragments in the head) may not be eligible. - Discussion of Expectations
We explain how many sessions you’ll need, how long each session lasts, and what kind of results you might expect.
Your First Day of TMS Therapy: Mapping & Calibration
Your first TMS session is a bit longer than the others because it includes a process called “mapping.” This step allows us to identify the exact location in your brain — typically the left dorsolateral prefrontal cortex — where treatment will be most effective. Using gentle magnetic pulses, we determine the correct position and intensity settings tailored to your unique brain activity. Mapping ensures that every session targets the precise area responsible for mood regulation. Once completed, future treatments are quicker and follow the same customized settings, providing consistent, effective stimulation for the best possible results throughout your TMS therapy.
The Motor Threshold Test
During the mapping process, we determine your “motor threshold” — the lowest magnetic pulse strength that causes a slight twitch in your thumb or fingers. This response tells us we’ve reached the part of the brain that controls movement, which serves as a reference point for treatment. Identifying your motor threshold is essential because it allows us to customize the stimulation to your brain’s unique sensitivity. Using the correct level of magnetic energy ensures that the pulses are strong enough to activate the targeted brain cells for mood regulation, while remaining safe and comfortable throughout your TMS therapy sessions.
Finding the Target Area
Using the results from your mapping session, we pinpoint the exact brain region that will benefit most from TMS therapy — typically the area linked to mood regulation. At Palmier TMS & Behavioral Health, we take precision seriously. Our team uses advanced coil positioning techniques to ensure the magnetic pulses are delivered to the exact location identified during mapping. This accuracy is crucial for maximizing the effectiveness of your treatment while keeping it safe and comfortable. By combining personalized settings with precise targeting, we give you the best possible chance for meaningful, lasting improvements in mood and overall well-being.
What Daily TMS Sessions Are Like
After the initial brain mapping is complete, your TMS sessions become quick, comfortable, and part of a regular routine. Mapping is a one-time process that identifies the exact location and stimulation level needed for your treatment. Once this is set, each daily session is streamlined and personalized to you.
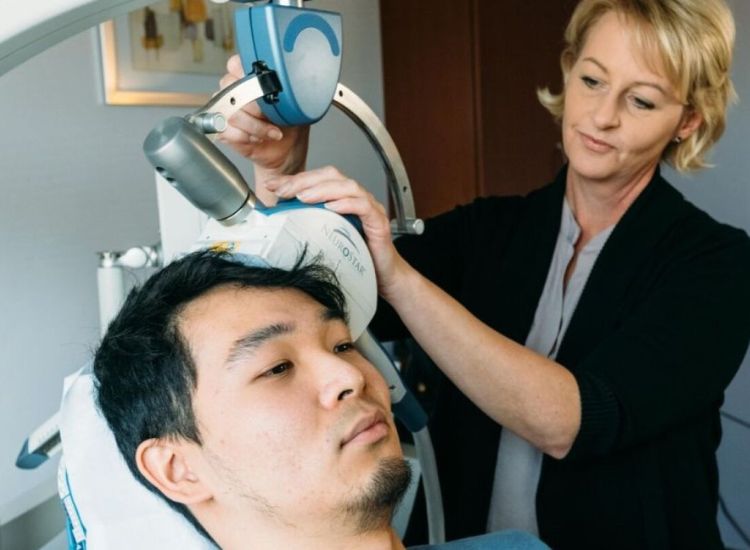
When you arrive for a session, you’ll be seated in a comfortable chair, and the TMS device will be positioned precisely where it was mapped during your first appointment. The treatment involves delivering gentle, repetitive magnetic pulses to your targeted brain area. You may hear a clicking sound and feel a light tapping sensation on your scalp, but the procedure is generally well-tolerated and does not require anesthesia or sedation.
Each session typically lasts 20–40 minutes, and you can immediately resume normal activities — whether that’s going back to work, running errands, or enjoying time with loved ones. Most patients attend sessions five days a week over several weeks, allowing the brain to gradually build healthier communication pathways.
Over time, these short, consistent sessions can lead to lasting improvements in mood, energy, and overall mental well-being, turning TMS into a comfortable part of your path toward recovery and emotional stability.
Here’s what a typical treatment day looks like:
- Check-In
You’ll be greeted by our friendly staff. We’ll ask a few quick questions about your sleep, mood, and whether you’ve noticed any side effects. - Seating & Setup
You’ll sit in a cushioned treatment chair. We position the magnetic coil over the treatment spot on your scalp. - Stimulation Time
The TMS machine delivers rapid magnetic pulses in short bursts. Sessions usually last 20–30 minutes. You’ll hear a clicking sound and feel gentle tapping against your scalp. - After the Session
You can drive yourself home, head to work, or carry on with your day — no downtime required.
Side Effects and Safety Profile
Most patients tolerate TMS very well. Possible side effects include:
- Mild scalp tenderness
- Light headache (usually relieved by over-the-counter pain medication)
- Temporary twitching of facial muscles during stimulation
These usually improve after the first week of treatment. TMS does not cause memory loss or systemic side effects like many antidepressants do.
The Timeline: When to Expect Results
TMS works gradually. Some patients begin feeling better in as little as 2 weeks, while others may take 4–6 weeks to notice significant changes.
At Palmier TMS, we check in regularly to:
- Track your mood scores
- Adjust treatment settings if necessary
- Provide encouragement and support
Life During TMS Therapy: Tips for Success
While undergoing TMS, here are a few ways to maximize your results:
- Stick to your schedule: Consistency is key to treatment effectiveness.
- Maintain healthy habits: Sleep, nutrition, and light physical activity all support brain health.
- Communicate openly: Let your provider know about any changes in mood, energy, or side effects.
- Stay engaged in therapy: Many patients benefit from continuing talk therapy during TMS.
Life After TMS: What Happens Next
After you complete your course (usually 30–36 sessions), we’ll discuss your next steps:
- Maintenance sessions — some patients schedule occasional follow-ups to maintain progress.
- Therapy & lifestyle support — ongoing counseling, exercise, and stress management help sustain results.
- Regular check-ins — we’ll monitor your well-being over time.
Many patients report:
- Renewed motivation
- Better relationships
- Improved work performance
- Greater enjoyment of life
Patient Story: A Day in the Life of “Anna”
To protect privacy, this is a composite of real experiences shared by our patients.
Anna, a 42-year-old teacher, had battled depression for over a decade. Medications helped only partially, and side effects left her exhausted. After her evaluation at Palmier TMS, she began a 6-week course.
By week 3, she noticed she was waking up with more energy. By week 5, her colleagues commented on her brighter mood. After completing TMS, Anna described feeling like “the fog had finally lifted.” She continued with therapy and made lifestyle changes to sustain her progress.
Frequently Asked Questions (FAQs)
Q: How long does each TMS session take?
A: Around 20–30 minutes per day.
Q: How many sessions will I need?
A: Typically, 5 sessions per week for 6–8 weeks.
Q: Does TMS replace medication?
A: Not always — some patients can reduce medications, while others use both treatments.
Q: Can I drive after TMS?
A: Yes — there’s no sedation or cognitive impairment.
Q: Is it covered by insurance?
A: Most major insurance plans cover TMS for treatment-resistant depression, but pre-approval may be required.
Conclusion
Starting Transcranial Magnetic Stimulation (TMS) therapy can feel like a big decision — but it’s a decision filled with hope. At Palmier TMS & Behavioral Health, we’re committed to guiding you every step of the way, ensuring you feel comfortable, informed, and supported from your first evaluation to your final session.
TMS is more than just a treatment for reducing symptoms of depression. By gently stimulating specific areas of the brain, it helps restore healthier communication between nerve cells, supporting long-term mood stability. Our goal is to help you not only feel better but also regain the energy, focus, and emotional resilience to fully engage in life again.
With a personalized care plan, compassionate providers, and a proven, non-invasive approach, TMS offers a new path forward. It’s not just about managing depression — it’s about reclaiming your well-being and building a brighter, more fulfilling future.
If you’ve tried traditional treatments for depression without lasting relief, don’t give up. TMS may be the breakthrough you’ve been waiting for.
Palmier TMS & Behavioral Health — Contact Information
Phone (Call or Text): 314-697-4867
Hours: Monday–Friday, 9 AM–5 PM (and by appointment)
📍 Chesterfield Clinic
112 Chesterfield Commons East Rd., Chesterfield, MO 63005
📍 Richmond Heights Clinic
1505 S Big Bend Blvd, Richmond Heights, MO 63117
📍 Osage Beach (Ozarks) Clinic
5721 Osage Beach Parkway, Suite 300, Osage Beach, MO 65065



