History of TMS (Part 3)
Evolution of TMS Devices Over Time
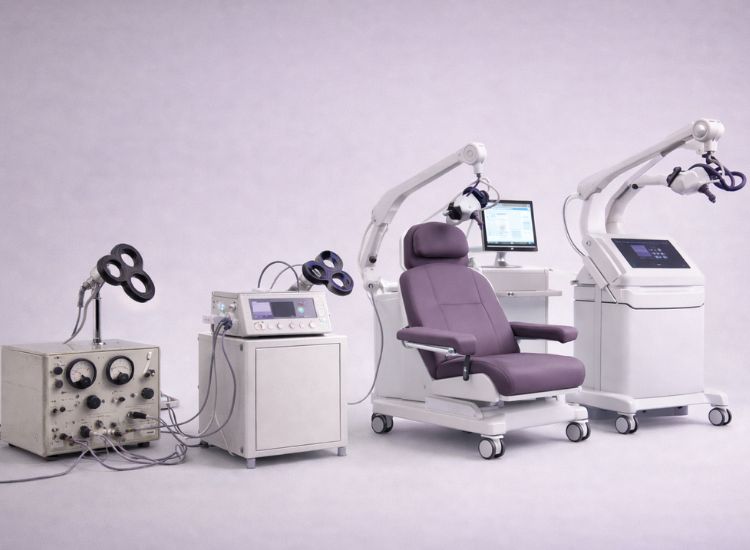
After Dr. Anthony Barker’s pioneering work in 1985, transcranial magnetic stimulation (TMS) underwent significant technological advancements that transformed it from an experimental tool into a widely used research and clinical device. While Barker’s initial TMS machine proved that magnetic fields could safely stimulate neurons, early devices were large, inefficient, and limited in functionality. Over the next decades, engineers and neuroscientists worked to refine TMS technology, improving coil designs, power sources, targeting precision, and safety protocols.
This section explores the evolution of TMS devices, focusing on the major advancements that expanded its applications in neuroscience and medicine.
Early TMS Devices (Late 1980s – 1990s): Expanding Research Capabilities
The first generation of TMS machines following Barker’s invention were designed primarily for scientific research, helping neuroscientists map motor pathways and study brain function. However, these early devices had several limitations:
- Single-pulse stimulation only—no ability to deliver repeated pulses for sustained effects.
- Bulky capacitor banks that required significant recharge times between pulses.
- Limited coil designs that lacked precision in targeting specific brain regions.
Despite these constraints, early studies demonstrated that TMS could be used to non-invasively explore brain function, leading to a surge in interest from the neuroscience and neurology communities. Researchers sought to improve coil designs and power systems to enhance TMS’s effectiveness.
Advancements in Coil Technology (1990s – 2000s): Increasing Precision
A major breakthrough in TMS evolution came with the development of more sophisticated coil designs, allowing for greater precision, efficiency, and comfort during stimulation.
1. The Figure-Eight Coil (Early 1990s)
- One of the first major improvements, this design replaced the original circular coil.
- The overlapping loops created a stronger, more focused electric field, improving spatial accuracy in stimulating specific brain regions.
- Impact: Allowed researchers to study localized brain function rather than stimulating large, diffuse areas.
2. The Double-Cone Coil (Mid-1990s)
- Designed to stimulate deeper brain structures by increasing the magnetic field penetration.
- Used in early experiments studying motor pathways and connectivity between the cortex and deeper brain areas.
- Impact: Enabled scientists to explore more complex neural circuits beyond just the outer cortical layers.
3. Liquid-Cooled Coils (Late 1990s – Early 2000s)
- As TMS devices became more powerful and efficient, coils began overheating during prolonged stimulation sessions.
- Liquid-cooled coils were developed to maintain optimal performance while allowing for longer treatment sessions.
- Impact: Improved patient safety and allowed for more extensive clinical trials.
These coil innovations laid the groundwork for modern TMS devices, enabling researchers and clinicians to target specific areas of the brain with greater precision.
Improvements in Power Supply and Pulse Control (2000s – 2010s)
Another major area of development was power management and pulse generation. Early TMS machines required large capacitor banks that limited the frequency of stimulation and required long recharge times.
1. High-Frequency Pulse Generators (2000s)
- Enabled rapid stimulation sequences that allowed researchers to modulate neural activity over time.
- Impact: Opened the door for studies on brain plasticity, memory, and cognition.
2. Programmable Stimulation Patterns (2010s)
- Modern devices introduced programmable pulse sequences, allowing researchers and clinicians to customize stimulation based on patient needs.
- Impact: Led to more precise and personalized treatment protocols.
These improvements expanded TMS applications, making it more effective for both research and therapeutic use.
Enhancing Targeting Precision: Neuroimaging Integration (2010s – Present)
One of the biggest advancements in TMS evolution was the integration of neuroimaging technologies to enhance targeting precision. Early TMS devices relied on external landmarks to determine coil placement, but this approach was imprecise and varied between individuals.
1. MRI-Guided TMS (2010s – Present)
- Functional magnetic resonance imaging (fMRI) allowed for real-time brain mapping, helping clinicians identify and target specific neural circuits.
- Impact: Ensured consistent and repeatable stimulation across patients, increasing clinical reliability.
2. EEG-TMS Integration (2010s – Present)
- Electroencephalography (EEG) is now used alongside TMS to monitor brain activity in real time.
- Impact: Allows researchers to adjust stimulation parameters dynamically, leading to more precise and individualized brain modulation.
These innovations have transformed TMS into a tool for personalized medicine, ensuring greater efficacy in both research and clinical settings.
The Shift from Laboratory to Clinical Use
Throughout the 1990s and early 2000s, TMS was primarily a research tool used to explore brain function and neural plasticity. However, as technology improved, TMS became a viable clinical treatment.
1. Standardized Safety Guidelines (2009 – Present)
- Rossi et al. (2009) published comprehensive safety guidelines outlining best practices for TMS use in clinical and research settings.
- Impact: Provided the foundation for regulated clinical trials and FDA approvals.
2. Expansion of Clinical Trials (2010s)
- As TMS devices became more advanced and precise, researchers began testing its therapeutic potential for neurological and psychiatric disorders.
- Impact: Set the stage for FDA-approved applications in depression, migraines, and OCD.
These advancements enabled TMS to transition from a neuroscience research tool to a standard clinical therapy, bringing it into mainstream medical practice.
Conclusion: The Evolution of TMS Devices
Since its invention in 1985, TMS technology has undergone remarkable advancements, transitioning from a basic experimental tool to a precise, widely used clinical device. The evolution of coil designs, power sources, safety protocols, and neuroimaging integration has allowed TMS to become a mainstream technology in neuroscience and medicine.
Thanks to decades of continuous innovation, TMS remains at the forefront of neuromodulation, with endless possibilities for future applications.
Sources:
- George, M. S., Wassermann, E. M., Kimbrell, T. A., et al. (1997). Daily repetitive transcranial magnetic stimulation (rTMS) improves mood in depression. NeuroReport, 8(6), 1213-1217. https://pubmed.ncbi.nlm.nih.gov/8547583/
- Levkovitz, Y., Isserles, M., Padberg, F., et al. (2015). Efficacy and safety of deep transcranial magnetic stimulation for major depression: A prospective multicenter randomized controlled trial. World Psychiatry, 14(1), 64-73. https://pubmed.ncbi.nlm.nih.gov/25655160/
- Rossi, S., Hallett, M., Rossini, P. M., & Pascual-Leone, A. (2009). Safety, ethical considerations, and application guidelines for the use of transcranial magnetic stimulation. Clinical Neurophysiology, 120(12), 2008-2039. Available at: https://pubmed.ncbi.nlm.nih.gov/19833552/
- Fox, M. D., Buckner, R. L., White, M. P., et al. (2012). Resting-state networks link invasive and noninvasive brain stimulation across diverse psychiatric disorders. Proceedings of the National Academy of Sciences, 109(26), 17510-17515. https://www.pnas.org/doi/10.1073/pnas.1405003111